Pre-departure:
The process to organize an international elective requires careful planning, consideration and most importantly, administrative skills.
Once I got in touch with Charité’s paediatric neurosurgery department in November 2017, I had to fill out many administrative forms that took months to complete. I needed to get a complete physical exam have Hepatitis A and B vaccinations (with records and proven adequate titres), an HIV test, a combination vaccination booster and records of having had these same vaccinations a baby. I would advise getting these done as soon as possible, as the Hepatitis vaccinations are done on a 6-month schedule and then another 4 weeks need to pass before your next vaccination can be administered. My vaccines were finally completed in May 2018 (and I was due to leave in July 2018). Make sure you check the health or administrative regulations of the University at which you are applying well in advance.
In terms of applying for my visa, Germany forms part of the Schengen state, and thus I needed to get a Schengen visa. Because I was considered to be “working”, I needed to apply for a business (and not just tourist) visa. This is more expensive, so be sure to budget for it, as the difference is about R500. I would also advise booking your flights about 4-5 months in advance, as airlines hike their prices up weekly (especially if you go during their heavy tourist season, as I did). In terms of organizing insurance, you don’t need to take the travel insurance that is offered by your travel agent. I bought travel insurance from the insurance company that insures our family’s assets and it came to about half the originally quoted price by the travel insurance. Also, make sure your travel insurance is for “business” and not just “tourism” – another hidden cost you might not have budgeted for.
When it came to organizing accommodation, I looked on multiple websites – especially ones that catered to students. The two that were the most successful were ErasmusU.com and wg-gesucht. These sites are quite well-trusted and have credited reviews. They also put you directly in touch with the person who is letting out their room for the summer. On that note, you will need a letter of their confirmation of the nature of your trip, their address and a copy of their passport to apply for your visa.
Retrospectively, I wish I hadn’t decided on a destination so late, so that I had more time to gather all my documents in a more organized way. I was also very lucky that I already had a passport, and had already applied for a Schengen visa in the last 2 years, and this sped up my visa acquisition.
Experience at Host University:
Charité in Berlin is the largest medical university Hospital in Europe, with 4 campuses (hospitals that act as teaching facilities too. Across the 4 campuses, Charité sees 660 000 outpatients and 140 000 inpatients a year – more than any other University Hospital in Europe. To put it into perspective, Berlin has a population of 3.45 million people, equivalent to that of the entire Western Cape. Tygerberg has 107 000 admissions per year, and sees more than 500 000 outpatients.

The Paediatric Neurosurgery (PNC) unit is situated at the Virchow Campus, situated about 5 km outside of the city centre. I took 2 trains to get to hospital every morning, a commute that took about 20 minutes. The Virchow Campus is built in a “pavilion”-style, with the wards or “stations” on either side of the Mittealle – a street that has a garden with trees and benches where patients can visit with their families.
Every morning meeting was spent planning the surgeries for that day. They make use of a lot of technology that is not yet available in the state sector here. For example, one of the surgeries I observed was done with a 3D exoscope – a cross between microsurgery and an endoscopic procedure. It was literally watching brain surgery in 3D.
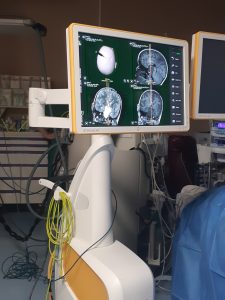
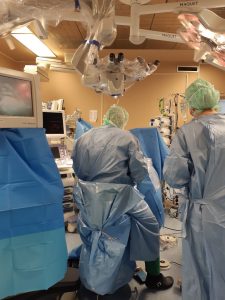
The atmosphere of the morning meetings was quite light – always done over coffee and breakfast. This is a big contrast to the environment in any hospital in South Africa, as oftentimes doctors feel guilty for eating in front of patients, as for many of our patients, hospital may be where they receive their most regular meals compared to their living situation. In the same vein, doctors never have to make decisions with the patient’s socio-economic conditions in mind. In Germany, the wait time is about 4-6 weeks for elective surgeries, whereas at Tygerberg the average wait time is around 9 months. Their waiting times at the outpatient clinic are also very short as they have set appointment times (like a private GP) and they have the clinic every week day, whereas it is done once a week at Tygerberg. They see around 20 patients a day in the clinic, where Tygerberg sees between 90 – 120 patients on the single clinic day.
In Germany, the surgeons also make decisions based on aesthetics and convenience a lot of the time, rather than cost. For example, they don’t like the aesthetic look that skin-clips (staples) leave, so they close with an organic glue that costs €250 per tube, and they use at least 2 tubes per surgery. Here in South Africa, we could never justify that kind of expense. Their record-keeping system (such as patient charts and notes) is all done digitally – and the computer generates graphs and figures that make it very easy to see a trend in e.g. blood pressure or temperature. It also ensures that no files ever go missing, and that everyone is accountable to keeping the charts updated.

In terms of my free time, I spent a lot of my time in museums, art galleries and outdoors. As it was summer, I wanted to be in my flat as little as possible and spent as much time as I could in parks, flea markets, outdoor concerts and open-air movies. Sundays in Berlin are spent in parks first at their open-air markets, then with families and friends – either reading, having a picnic or tossing a frisbee.
Return to Stellenbosch:
In Germany, my best moments definitely came from seeing what a difference a “near-perfect” healthcare system can make in terms of patient-care, -outcomes and doctors’ level of job satisfaction. There were obviously things that they as doctors complained about, like long waits between surgeries, but they were so focused on the surgery – the thing they were trained to do. They didn’t have to be the social worker and transport manager and administrative clerk.
On the opposite side of this though, we may not have the luxury of breakfast meetings and 15 specialised plasters that essentially could all do the same job, but I think it makes South African doctors and healthcare professionals more innovative and more compassionate. We may not have the luxury of time, but that doesn’t mean we compromise our patient-centered care principles for the sake of saving time. It means we work smarter, and (in my perhaps still very naïve opinion) work better, because we don’t have all the conveniences that would make our jobs easier.
I think my international experience broadened my mind to what is possible in medicine and to a very different way of approaching problems and doing surgeries. There are definitely lessons that I will take away from the experience besides the new techniques, such as maybe taking the extra effort to consider the aesthetic and psychological effect of brain surgery on a patient.
One of the unexpected skills that I had the opportunity to work on despite it not being part of my elective outcomes was the under the “Attitudes/Values” heading of the Profile of the Stellenbosch Graduate: “the willingness to set a positive example regarding social responsibilities and obligations”. The Professor who was head of the department asked me to do a presentation on what medicine is like in South Africa, what my university is like, why I want to do neurosurgery and what my country is like as whole. I was honest. I said South Africa is still very much struggling to reach the level of unification that Berlin has managed to achieved, and I elaborated on some of our socio-economic issues. After the presentation, they said that their ways of thinking had been challenged by my presentation, but also that they had such great respect for the doctors that work in South Africa, because of the unique challenges we face every day.
At the end of the day, I don’t think paediatric neurosurgery or first world medicine is where I’m meant to be, I’m so grateful for the experience and the opportunity to find that out. I would definitely consider moving to Berlin. I fell in love with the city, and would definitely love to work there for a short while and learn what I can from their systems, and try to find a way to incorporate it here at home.
But I think South Africa is where my heart is truly, and where, one day, my skills can be put to the best use and create the most change. Surrounded by dynamic, innovative, compassionate doctors that advocate for their patients like non-others, and actually continue to push the boundaries of what’s possible with what we have.